COVID19
AIIMS chief warns India about surge in fungal infection in COVID-19 patients
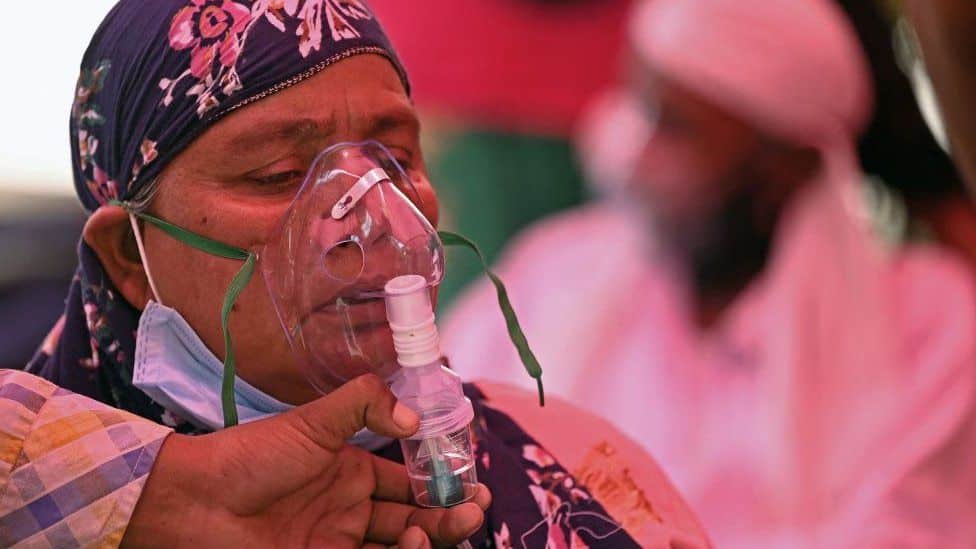
With a pattern emerging of more than 90% of mucormycosis patients being diabetics, AIIMS director Dr Randeep Guleria has emphasized the urgent need to control and monitor sugar levels in COVID-19 patients. He also warned about a surge in mucormycosis, which is a rare fungal infection, across India.
Speaking during a session of a clinical excellence programme to guide state centres of excellence and districts in clinical management protocol, Dr Guleria said data links the current increase in mucormycosis cases with diabetes and steroid intake. He highlighted that doctors from Gujarat have reported more than 500 cases of the fungal infection only from government hospitals.
“Hospitals in Gujarat have set up more than one ward just to manage patients with mucormycosis and are now forming combined teams with infectious disease specialists, ENT surgeons, neurosurgeons and plastic surgeons to operate upon these persons,” the AIIMs chief said. “Almost of the mucormycosis patients had taken steroids. More than 90-95% were diabetics. COVID itself leads to lymphopenia, therefore, predisposing patients to opportunistic fungal infections.”
Dr Guleria pointed out that steroid intake can lead to a spike in blood sugar levels. Unlike the first wave of the pandemic, he said doctors are now seeing the fungal infection develop even in patients who are battling COVID-19. “We are seeing mucormycosis happening now even when the patient is COVID-19 positive. During the first wave, it would occur later on. Now we are having two sets of patients – COVID patients with mucormycosis who we are keeping in the COVID ward, and those who become COVID negative and continue to have mucormycosis. And the management strategy becomes even more challenging because of these two sets of patients.”
Also Read: Desperate people turn to black market for critical COVID-19 drugs and oxygen supplies
The AIIMS chief said focus has to be on the preventive aspects – judicious use of steroids and good control of diabetes. “Among the cases in Gujarat, about five to 10% patients who developed it were not admitted in hospitals,” he said. “They were in home isolation and started steroids at home, and then came to hospital with features of mucormycosis.”
Dr Guleria said such cases will be seen in many parts of the country as steroid intake has increased during the second wave of infections.









































Pingback: State governments should report COVID-19 cases transparently without feeling any pressure, says Prime Minister Narendra Modi.